| INTRODUCTION | ||
| As I came to my senses, to some minimal extent, on the morning of Sept 10, 2005, there were several paramedics gathered around the bed. Normally, that might be cause for alarm, but at the time it didn't strike me as anything out of the ordinary (which should also have been cause for alarm). After several rounds of questions, most of which I don't remember, I was able to tell the paramedics what year it was (I couldn't get the day or month, but unfortunately I could name the president, something I wish I had been able to forget). I spent the rest of the day in the UNC Hospitals ER, being assayed and having Carol (my wife) describe what had happened, again and again (to me - she only had to tell the ER staff once for them to get it). I'd had a seizure . An MRI of my brain showed a cyst in my right temporal lobe. There was some "stuff" around the cyst (Fig. 1A). Could have been inflamation from the seizure, but it was unchanged six weeks later. The seers were undecided between low-grade glioma or scar tissue from an old injury (a couple of candidate accidents come to mind, as it were). We eventually decided to have it removed (the lesion, not the brain...though a chunk of brain went with it) by the skilled people at the Tisch Brain Tumor Center at Duke. |
||
| RESULTS | ||
| Surgery was scheduled for the morning of March 9, 2006. A Carolina guy going to Duke for surgery is one thing, but doing the weekend of the ACC basketball tournament seemed pretty brave. As it turns out, most of the staff there seemed to be Tar Heel fans, judging by their pins and earing (alas, Duke Medical has since implemented a policy that forbids staff from wearing anything that promotes any sports team). The surgeon, Dr. Allan Friedman (he who two years later operated on Sen. Ted Kennedy) removed a chunk of my brain (Fig. 1B). He reckoned it to be about "two walnuts worth". [Instead of the surgeon holding out his hand and saying, with due authority, "Scalpel!", I picture him saying, "Melon baller!"]. He knew going in that the tumor was not going to be "a cherry in a Jell-O bowl", so he had planned to remove a section of mostly "normal" brain, and probably wouldn't get the entire lesion. Dr. Friedman (more likely a medical student or intern) then stitched my head up nicely (Fig. 2A). I went home the following Saturday (March 11), released into Carol's care. She did a great job, even while navigating through her first semester on the faculty of the Department of Art (visit her DoA page). |
||
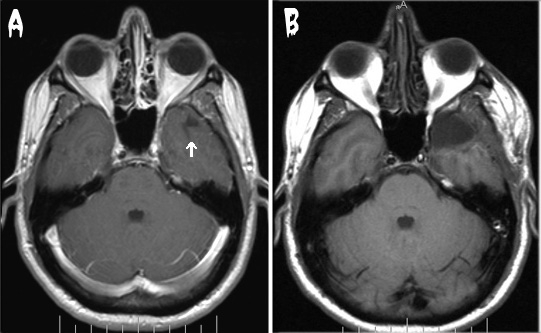 |
Figure 1. MRI sections from before (A) and after (B) my brain surgery. The arrow in (A) indicates the suspect area in the front of the right temporal lobe (the arrow was Photoshopped in - it is not really in my head). The dark area is a cyst, and the whitish stuff surrounding it (the stuff you can't really see here) is the problem. In (B), this area is gone, along with some stuff around it that I guess I didn't really need anyway. Note: The shape of my head did not change as drastically as these images show. The MRIs were done on different machines with (perhaps) different software, and the sections are somewhat offset from one another. However, the swelling of the right jaw muscle in the "after" photo is real (five weeks after surgery). Three months later my glasses still left a dent in the side of my head. | |
 |
||
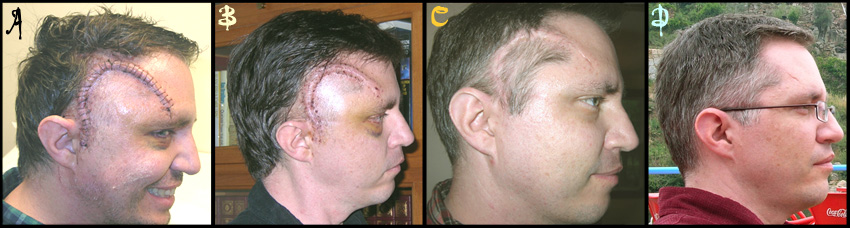
| Figure 2. Fading of the scar. This series shows the progression of healing as assayed by appearance and disappearance of the scar. A. One week post-surgery. B. Two days later, after the stiches were removed (and I was able to wash my hair). C. Three weeks after surgery. D. Three months after surgery, while cruising on the Duoro River in Portugal's Port wine region. Sadly, the scar is now nearly invisible. |
||
| CONCLUSION | ||
| The determination of the pathologist (Supplemental Online Material) is that I had a dysembryonic neuroepithelial tumor (DNT or DNET). People in the know say that if you're going to have a brain tumor, that's the kind to have. It means I shouldn't require any additional treatment (for this, at least) except an MRI in a year and remaining on anti-seizure meds until then. It is very likely that there will be no more seizures (none attributable to the DNT, anyway; those caused by faculty meetings or my lab are unpredictable). After March '07 I will be forced to find a new excuse for my behavior. The surgery was actually had a pretty minor effect on my lifestyle. I was home for six weeks, then back part time for six weeks. People say it takes about a year to really recover from surgery. I think that was true for me, but it took a long time to realize that. Every few months I'd say, "Well, I think I'm 100% now, but two months ago I definitely wasn't". On the other hand, the anti-seizure drugs had a major effect. I was on Dilantin from the day I had the seizure (Sept 10 '05) until six weeks after the surgery (late April '06). Dilantin made me stupid, like being on 5X antihistamines. Dr. Friedman recommended I switch to something less strong, so my neurologist at UNC, Dr. Aucutt-Walter, put me on Keppra. As I tapered off Dilantin I found myself able to think again. I even started to have ideas for the lab! Unfortunately, the Keppra made me mean. During my months on Keppra I defintely burned a few bridges with journal editors (who no doubt deserved it). |
||
| SUPPLEMENTAL ONLINE MATERIAL Pathologists' report |
||
|
||
| POSTSCRIPT |
||
| On April 23, 2007, I had the one-year post-surgery MRI, followed the next day by a consultation with Dr. Friedman: Surgeon: You remember that I didn't take out any of your memory. Me: No, I don't remember that. Surgeon: Well, we don't even know if it works. Me: Huh? Surgeon: Your memory. It might be all on the other side. Me: Huh? Surgeon:Before surgery, I talked about possibly removing part of your hippocampus, which could lead to some short-term memory deficits, but I didn't need to do that. Anyway, something changed on your MRI since a year ago. Me: You mean my brain grew back? Surgeon: No, nothing like that. It doesn't really concern me, but I think we should wait and have another MRI in six months. Me: So, I suppose that means I should stay on the anti-seizure meds until then? Surgeon: That would be my recommendation. Well, it's been nice cutting you. See you in six months. |
||
| In September, 2007, I had another MRI. It looked good, so I also had a sleep-deprived EEG. No problems there either. I decided not to go off the anti-seizure meds just yet, since Carol and I were planning a trip to Mali in November, and I didn't want to risk having a seizure in Timbuktu. In late December, 2007, I tapered off the Keppra, and have had no further problems (except that my sense of humor seemed to return). |
||
| In December, 2012, I had another surgical procedure: removal of about 12" of terminal ileum and a few inches of colon. Not as high on the list of favorite organs as the brain, which is very close to the top. This procedure took much longer than brain surgery (4 1/2 hours vs. 90 min), required a much longer hospital stay (5 days vs. 2 days), but much faster recovery. Seems to have, at least for the time being, cured the Crohn's disease I've had for 33 years. In response to numerous pleas, I am not posting photos. | ||

